Keratoconus
What Is Keratoconus?
It's a Manageable Corneal Condition
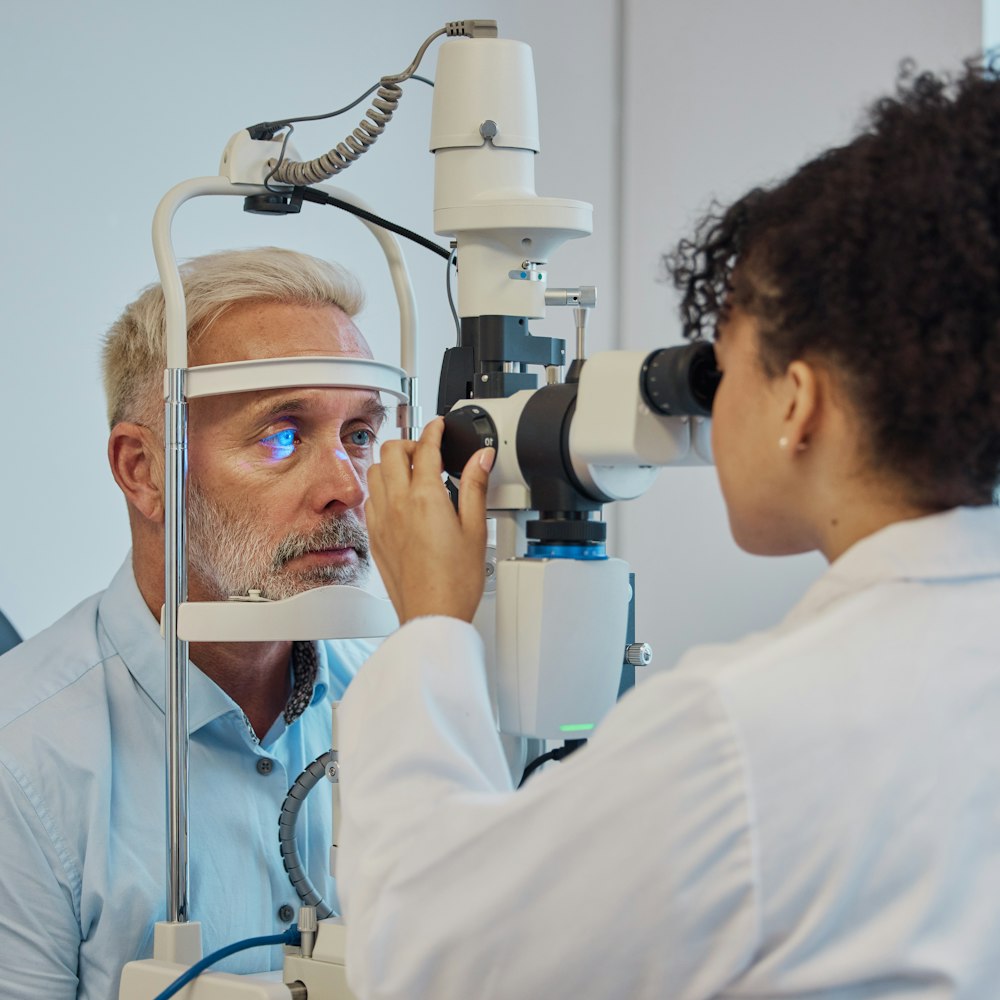
Keratoconus is a corneal condition that typically starts to develop in patients between puberty and the onset of their thirties. It affects the shape of your eye, making it more cone-like. Keratoconus causes the cornea to thin, and can eventually lead to vision loss.
Because it's progressive, you'll want to find treatment as soon as possible, such as special contact lenses or eye surgery.
Though many of our Dallas patients have already been diagnosed with keratoconus by their primary eye care doctor and have been referred to us for surgical treatment, we can also help those at the beginning of their treatment journey.
If you suspect that you may have keratoconus, we can diagnose and treat your corneal condition.
How Keratoconus Affects the Shape of Your Cornea


By Finding Care for Keratoconus You Can Stall the Symptoms
Light Sensitivity
Fuzzier Vision
Corneal Scarring
The earlier you're diagnosed, the less chance keratoconus has to worsen. You can refrain from eye rubbing, which may play a role in the condition. It's also often easier to treat using custom contact lenses or glasses.
Though being diagnosed with keratoconus can be stressful, you have the power to protect your cornea. By visiting Cornea Associates of Texas for care, you can do your part to maintain healthy vision.
From Fort Worth to Dallas Texas Patients Appreciate Our Eye Doctors
Dr. Comstock quickly assessed my problem, explained my treatment options, and frequently monitored my progress to make sure I was steadily improving. She patiently answered any questions I had and was compassionate in her care.
View on GoogleAbout 25 years ago I needed to see a cornea specialist in D/FW, and I was referred to Dr Beebe. He's still my eye doctor. He does a terrific job.
View on GoogleNon-Surgical Treatment For Keratoconus
At earlier stages, many cases of keratoconus can be managed simply with custom eyeglasses or contacts. If that's not the case for you, don't stress — you're in good hands at our practice.
Local optometrists often refer patients out to our office when they cannot treat them with specialized glasses lenses or contact lenses alone.
Check Out Our eBook To Learn More!
Will Insurance Help With My Treatment?
Like astigmatism and other conditions that impact your vision and eye health, keratoconus treatment is eligible for insurance coverage. Whether that includes contact lenses or surgery, your provider will likely help with a portion of the price. We accept most insurances and are a Medicare provider. We also accept financing.